
Marrow donor meets boy she helped saveBy Venita Jenkins
Staff writer

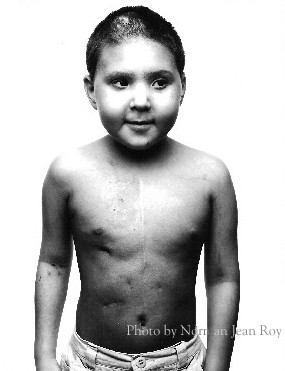
Annette Locklear visits with Matt Pearl, to whom she donated bone marrow in 2006.
PEMBROKE — Annette Locklear signed up to be a bone marrow donor when she was a high school senior. She never thought she would be called one day to save a life.
That call came in 2001, when a representative of the National Marrow Donor Program Registry told her she was a close match for a child in Missouri who suffered from a rare blood disorder.
Locklear, a teaching assistant at Deep Branch Elementary School, didn’t think twice about helping.
“If it was my child, I would want someone to help,” she said.
Locklear was honored for her gift of life on Mother’s Day weekend. She also met the boy, Matt Pearl, who received her bone marrow.
Diane Pearl, Matt’s mother, wanted to thank the people who gave her the greatest Mother’s Day gift — saving the life of her two children.
Matt, who is 11, and his 13-year-old sister Alex were diagnosed with Fanconi anemia, a rare blood disorder that leads to bone marrow failure. The disorder can affect the body’s organs, tissues and systems.
Locklear, who is 30, and a 40-year-old woman from Sweden named Catarina Lindstrom visited the Pearl family in Missouri last week.
“They gave me Mother’s Day every day,” Pearl said during a telephone interview from her home in Eureka, Mo.
Alex received bone marrow from Lindstrom during a transplant in May 2001.
Matt did not undergo his transplant until five years later. Pearl said Locklear’s tissue was a close match, but there was only a 50-50 chance that Matt would survive.
The family searched for five years to find a perfect match. They hosted bone marrow drives. Nearly 100,000 donors were added to the registry. But, they did not find a donor who matched more closely than Locklear.
“I can’t imagine searching for five years to find someone to save your child’s life,” Locklear said. “Diane told me they were hoping that I was still alive and I still wanted to donate because there wasn’t anyone else.”
During the search, Matt’s health started to deteriorate. The family asked the registry to contact Locklear so they could proceed with the transplant.
“Matt was getting critical. We had no choice,” Pearl said. “We could no longer keep them alive.”
Locklear went to Chapel Hill on July 14, 2006, to have bone marrow removed from her lower back. The next day, several thousand miles away in Minneapolis, Matt received her bone marrow.
“I know they say, ‘If it wasn’t for me.’ But it wasn’t me,” Locklear said. “The Lord had all that worked out years ago.”
Program rules
The children could not meet or communicate with their donors until a year after the transplant, and only with the donor’s consent.
Locklear checked in with a representative from the registry about Matt’s progress. It wasn’t until November that she heard from Pearl in an e-mail. Pearl expressed her gratitude and the desire to meet Locklear. They decided to meet in May.
Locklear said she was nervous about her trip.
“Once I got there, everyone was so nice, kind and loving,” Locklear said. “I felt like I was at home. I can say that was probably the best Mother’s Day for me. All our families were there together.”
Pearl felt a great sense of peace and comfort when she finally met Locklear and Lindstrom, she said.
“It was like I had known them forever,” Pearl said.
The children are healthier and happier, she said.
“Matt knows she gave him something special,” Pearl said.
Locklear received a necklace with a silver pendant with her initials on the front, along with Matt’s name and the date of the transplant on the back. She also was given a book filled with letters of thanks from friends and family, and stories about the children.
“I am just a working mother with two kids, but I had people come up to me saying, ‘You don’t know what you have done,’” Locklear said as she flipped through the book.
Pearl said it was hard to convey the family’s gratitude.
“To come full circle and to have them with us on Mother’s Day was such a great honor,” she said. “There is no way we can thank Annette and Catarina for saving the children’s lives. They think they did nothing. They answered a call. They got on the registry and did something we all need to do.”
Locklear said she now plans to become an advocate the bone marrow registry.
“I think people need to be educated about the process,” she said. “I think more people would sign the registry.”
Locklear said she would do it again. “Knowing what I know now, absolutely,” she said as she held her 2-year-old in her arms.
Staff writer Venita Jenkins can be reached at jenkinsv@fayobserver.com or (910) 738-9158.